What is claudication?
Claudication is pain, tiredness and weakness in the legs after walking a certain distance. Arteries carry oxygen and nutrients to the legs. During exercise the requirement for oxygen and nutrients by the muscles in the legs is increased. Normal artery is able to accommodate the increased demand by dilatation (increasing the calibre of the tube) and allow a greater amount of oxygen and nutrients to reach the muscles. In artery affected by atherosclerosis, the artery is narrowed or completely blocked and hence the amount of oxygen and nutrients supplied to the muscle is much reduced. When muscle is deprived of nutrients, it produces lactic acid by anaerobic metabolism and lactic acid accumulation in muscle causes pain.
The onset of the symptom is dependent on the severity of the arterial disease. In mild cases, the patient is able to walk a long distance (several km) before the onset of pain, however as the blood supply worsened, this distance is often reduced to 200 metres or less and eventually pain can develop even without exercise (rest pain). Rest pain usually affects the forefoot and toes. People with rest pain often need to dangle the foot over the edge of the bed or sleep in a chair to get relief. In extreme cases ulcer and gangrene can also develop. Claudication pain usually stops immediately upon stopping exercise. People affected do not need to sit down to get relief from the pain. Walking uphill and downhill can bring on the symptom earlier. Back problem from spine (spinal claudication) can present very similar to arterial claudication except that in spinal claudication, affected individual usually need to sit down or lean forward to get relief. Walking uphill is easier compared to walking downhill in spinal claudication. Spinal claudication usually takes more than 15 min to settle down, whereas pain from arterial claudication stop almost instantaneously after cessation of exercise.
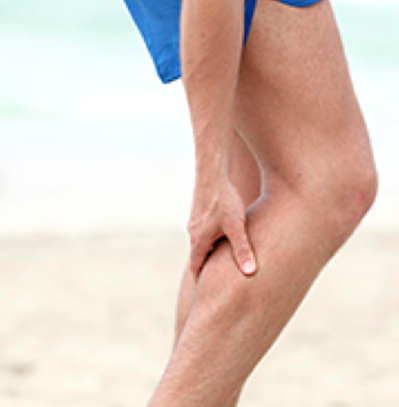
Figure 1: Calf claudication
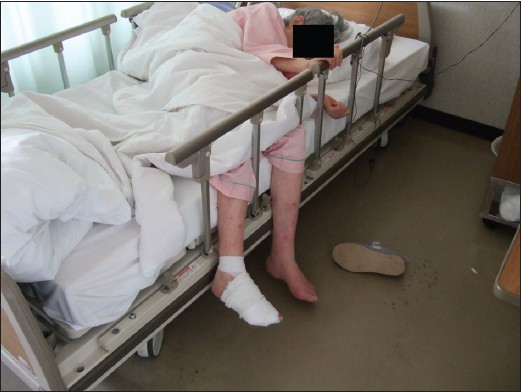
Figure 2: Rest pain and ulcer right foot (bandaged)- relief from dangling feet over edge of bed
Claudication is a serious symptom because people who have it are also at increased risk for heart attack and stroke. Normal artery is normally smooth and has no narrowing and able to allow blood to flow freely to deliver oxygen and nutrients to the tissue. Atherosclerosis, also called
“hardening of the artery” is build-up of plaque (waxy substance made up of cholesterol, muscle cells, fibrous tissue and calcium) in the walls of artery, narrowing and stiffening it initially and eventually causing complete blockage. Atherosclerosis is a generalized process and therefore it is likely to affect the leg arteries as much as the coronary arteries (heart) and the carotid arteries (brain). Early diagnosis allows risk factors modifications by lifestyle changes and medications.
Risk factors for atherosclerosis
- Age
- Gender- more common in male
- Family history of early stroke, coronary artery disease or leg artery blockage
- Smoking
- Obesity
- Hypertension
- Hyperlipidemia- high total cholesterol and low high-density lipoprotein (HDL) cholesterol are independent risk factors
- Diabetes- poor glycaemic control predispose to peripheral arterial disease
- Sedentary lifestyle
- Depression
Investigations
Your doctor will perform a thorough history and clinical examination collecting information on your symptoms, past medical history, current medications, smoking history, family history, blood pressure reading, and presence or absence of pulses and bruit (noise in the artery indicating narrowing) in different locations of the body prior to organizing for you to have radiology tests.
Radiological investigations
Ankle-brachial index (ABI)
This is a non-invasive method of detecting PAD. It is performed by measuring the blood pressure at the ankle level and compared that to the blood pressure at the arm level. The value of ABI and the probable severity of peripheral arterial disease (PAD) is summarised in Table 1 below.
| ABI | Diagnosis |
| >1.4 | Non-compressible arteries |
| 1.0-1.4 | Normal |
| 0.90-0.99 | Borderline |
| <0.9 | Peripheral arterial disease |
| 0.6-0.9 | Claudication |
| 0.3-0.6 | Rest pain |
| <0.3 | Impending gangrene |
Table 1 ABI value and the diagnosis and severity of PAD
The diagnostic value of ABI is limited in diseases that cause severe hardening of artery such as in advanced diabetes mellitus, renal failure and the very elderly due to inability to compress the artery, giving rise to an artificially high value. ABI is a strong marker of cardiovascular disease and is predictive of cardiovascular events and mortality. Artery in the toe (digital artery) is less likely to be affected by calcification and toe pressure measurement can be helpful in predicting likelihood of healing in situation where there is severe hardening of the artery at the calf and ankle level (tibial artery).
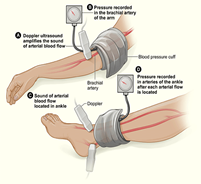
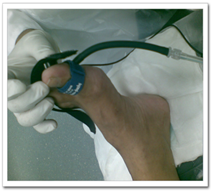
Figure 3: Measurement for ankle brachial index (ABI) on the left and toe pressure on the right
| Toe pressure (mmHg) | Healing |
| < 30 | Unlikely to heal |
| 30-60 | May or may not heal |
| > 60 | Likely to heal |
Table 2 Toe pressure value and the likelihood of ulcer healing
∗Patient with diabetes requires higher toe pressure to heal compared to patient without diabetes
Duplex arterial ultrasound
Colour duplex arterial ultrasound is non-invasive method that is often the first line investigation for peripheral arterial disease (PAD. It provides information on sites of stenosis or occlusion, and it can also provide information on the flow within the artery. The quantification of degree of stenosis by colour duplex ultrasound is based on Bernoulli’s principle or garden hose principles (Fig 5). Bernoulli’s principle states that as the speed of blood flow increase through the stenosis, this is accompanied by a decrease in arterial perfusion pressure distally. It is much like when you hold your thumb over the end of a garden hose. The pressure (potential energy) behind your thumb accelerates the water and so it squirts out the end of the hose. Once that potential energy is used to accelerate the water in the form of kinetic energy, all the potential energy has been converted to kinetic energy and this leads to a pressure drop beyond the stenosis. The disadvantages of duplex ultrasound are that it is highly operator dependent, poor quality images due to arterial calcification or bowel gas, and inability to provide complete anatomical information.
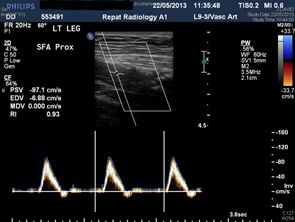
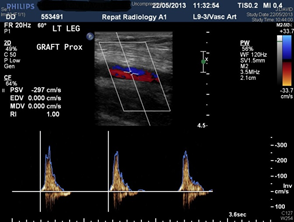
Figure 4: Normal artery flow on the left and high velocity flow across narrowing in the artery on the right (Peak systolic velocity 3X compared to adjacent segment)


Figure 5: Garden hose principle- Laminar flow on the left with no narrowing; turbulent and fast flow water jet from the narrowed nozzle
Computed tomography angiography (CTA) and Magnetic resonance angiography (MRA)
CTA and MRA are both non-invasive modalities of investigation used in investigation of PAD. Both provide good anatomical information but do not provide information on blood flow within the artery. These tests are often combined with Colour Arterial Duplex to allow planning of surgical intervention.
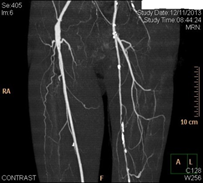
Figure 6 (CT Angiogram)
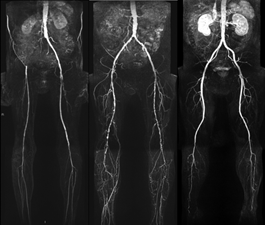
Figure 7 (MR Angiogram)
Digital subtraction angiography (DSA)
Digital subtraction angiography is usually performed at the time of surgical intervention to improve the blood supply to the affected artery. This is due to the invasive nature of the procedure requiring insertion of wire and plastic tubing (catheter and sheath) into the artery for performance of the procedure. Contrast dye is also necessary for the procedure and this may cause kidney damage. Other complications of DSA includes bleeding, false aneurysm formation and damage to the wall of the artery.
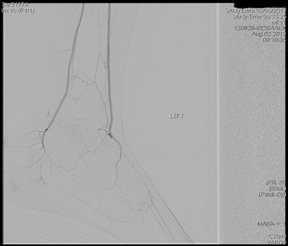
Figure 8 (Digital Subtraction Angiography)
Treatment
Lifestyle changes and medication
- Stop smoking
- smoking damages the artery
- smoking reduces the success of surgical intervention
- Blood pressure reduction
- aim 130/80 mmHg in patients with diabetes
- aim 140/90 mmHg in patients without
- Healthy weight and diet
- Ideal weight should be BMI <25 kg/m2 and waist circumference <94 cm in men (<90 cm in Asian men) or <80 cm in women (including Asian women).
- Consume a varied diet rich in vegetables, fruits, wholegrain cereals, lean meat, poultry, fish, eggs, nuts and seeds, legumes and beans, and low-fat dairy products.
- Avoid high salt intake and limit alcohol intake to ≤2 standard drinks per day
- Regular exercise
- National Heart Foundation of Australia recommended 30 minutes or more of moderate intensity physical exercise on most days of the week. This can be accumulated in short bouts such as 10 minutes sessions. The intensity of the exercise should be increased over time to obtain maximum benefit
- Antiplatelet (blood thinner) therapy
- aspirin or clopidogrel
- Clopidogrel has slight advantage over aspirin in preventing adverse cardiovascular event
- Clopidogrel is more expensive than aspirin
- Statin (Cholesterol tablet)
- Lipid profile target –total cholesterol <4mmol/L, HDL >1mmol/L, LDL< 2mmol/L, Triglycerides <2.0mmol/L
- Stabilizes atherosclerotic plaque- this is the most important property of statin. It prevent plaque rupture causing heart attack, stroke or sudden blockage of artery
- Improve lipid profile
Endovascular Intervention and Surgery
- The risks and benefits from intervention for peripheral arterial disease (PAD) need to be thoroughly considered and discussed with your vascular specialist before interventions. Intervention on artery at the level of the calf (tibial artery) carries a higher risk of complication than interventions for artery in the thigh (femoral or popliteal artery). Interventions on calf artery are generally only indicated in cases where there is rest pain, ulcer or gangrene whereas intervention in the thigh artery may be performed for lifestyle limiting claudication
- Balloon angioplasty and stenting form the backbone of endovascular interventions. These procedures are minimally invasive and performed from within the artery with a small cut in the groin usually. Recovery time is short and in hospital stay is generally limited to 1-2 days. The results from endovascular interventions are generally not as durable as surgical bypasses, however it has less associated morbidity and therefore is generally considered as first line treatment option for elderly patient with PAD
- Bypass surgery is the gold standard in improving the blood supply to the leg for peripheral arterial disease (PAD), however it carries with it significant morbidity and small risk of mortality (3%). It is usually performed on younger patients with good life expectancy. This operation also requires the patient to have good quality vein to use as conduit for the bypass. People who had their varicose veins stripped in the past do not generally have suitable vein to be used for the bypass
- Major amputation (below the knee or above the knee) is used as a last resort for patient with no option to improve the blood supply to the leg. It carries with it significant morbidity and mortality (25% in 1 month and 50% in 1 year). A small proportion (20%) of patient manages to walk with the aid of a prosthetic limb after major amputation.
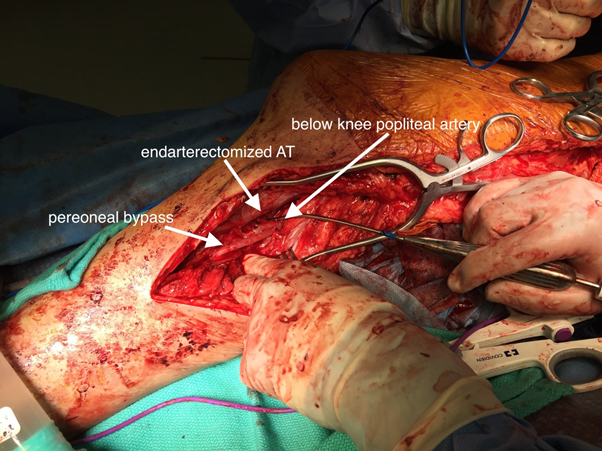
Figure 9: Femoral tibial bypass
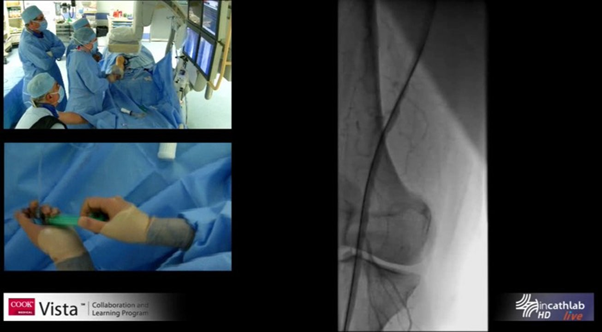
Figure 10: Endovascular procedure to improve blood supply to the leg